Introduction
Lung cancer is still the most common cause of malignancy related deaths in Jordan,(1) with most of the cases being discovered and
diagnosed in relatively late stages. Screening and early detection of lung cancer can increase the incidence of early stage tumors and will offer
better treatment options to patients. Diagnosing patients with lung nodules is a multi step process that ends in pathology department were the definite
histological diagnosis is made and confirmed.(2)
Many methods of obtaining histological diagnosis is present nowadays including Fiber
Optic Bronchoscopy, CT-guided Fine Needle Aspiration Biopsy (FNAB), open and Video Assisted Thoracoscopic Surgery (VATS). CT-guided FNAB had proven its
sensitivity and specificity in determining the histological diagnosis in lung nodules more than 7mm.(3) Apart of post FNAB
pneumothorax, it carries very low risk of complications as bleeding and infection. (4) In this retrospective study we reviewed the
data, CT-scans and X-rays of our patients in King Hussein Medical Center to evaluate the rate of pneumothorax and the contributing factors associated
with it.
Methods
This retrospective descriptive study was held at King Hussein Medical Center, Thoracic and Pulmonology Divisions between the period starting April 2013
and ending March 2014. Approval from the ethical committee was obtained to carry out the study. It included 105 patients who were diagnosed to have
lung nodule and/or nodules. All nodules more than 1cm were set to have CT-guided FNAB for histological diagnosis. All nodule/nodules regardless of
site, size, location and lung condition were included. Patients less than 14 years were excluded from the study. Data were collected from the
Radiological Department records, the Thoracic Division computerized data system and patients files. All CT scans and post FNAB chest X-rays were
reviewed from the PACS system of the Radiology Department by thoracic surgery specialist and a radiologist.
CT-guided FNAB were done as an inpatient procedure. All patients had their Complete Blood Count (CBC) tested and had their bleeding profile (PT, PTT,
INR) done at the same day of the procedure. All patient were kept fasting for four hours prior to procedure. The procedure was done in the radiology
department using a Siemens CT scan. Two
senior radiology consultants and two radiology specialists had done the procedure with no selection for patients per radiologist.
Technique of CT-guided FNAB was standard for all patients and operators. An 18-gauge needle size (Fig. 1) was used for all patients. The procedure
included positioning of the patient prone, supine or lateral according to lesion position so that there is a direct access to the nodule using CT
scanning (Helical Siemens CT scan), a metal marker was used on the chest wall to determine site of needle insertion followed by needle marking on the
chest wall and under CT scanning biopsy needle was inserted down to the nodule core under guidance followed by aspiration (Fig. 2). Patients were
observed for pneumothorax at two stages; the immediate stage on CT-scan table while performing the biopsy and depended on the CT slices to show the
presence or absence of pneumothorax, and it was done by the operating radiologist (Fig. 3). The late stage involved a standing chest X-ray four hours
post the biopsy to check for pneumothorax, and it was read by the pulmonologist on call. All patients were monitored in the ward post biopsy for
shortness of breath and respiratory distress.
All patients were given prophylactic dose of wide spectrum intravenous antibiotic half an hour prior to the procedure. Post procedure pain was managed
according to pain scale and according to hospital protocol in pain management.
All patients with negative post FNAB chest X-ray for pneumothorax were cleared for discharge from the hospital on the same day and followed in the
clinic as an outpatient bases. All patients with positive CT and/or Chest X-ray for pneumothorax were treated by thoracic surgeon on call in accordance
with The British Thoracic Society (BTS) guidelines for treating Pneumothorax and follow up accordingly in The Surgical Ward. After discharge the
patients were followed in the clinic one week later.
Continuous data are presented as mean ± standard deviation, categorical data are presented as frequency (percent).
Fig. 1:
An 18 gauge aspiration needle.
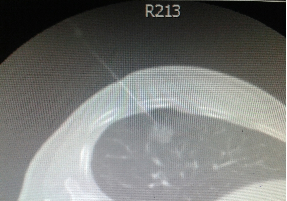
Fig. 2:
Needle taking biopsy under CT-guidance from lung nodule.
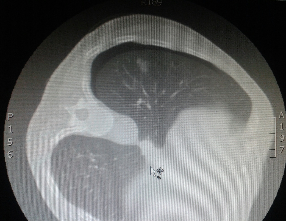
Fig. 3:
Pneumothorax as detected immediately on CT scan after fine needle aspiration.
Results
There were 83 males (79%) and 22 females (21%) who were included in this study. Their age ranged from 35 to 77 years and the mean age was 62±10.8 year.
Fifty three patients had their nodules on right side (50.4%), where left sided nodules were found in 52 patients (49.5%). The right upper lobe was the
most common site of nodules with 34 patients (32.3) (Table I). Almost two thirds of the nodules were peripheral and 19% of all patients had element of
lung emphysema; focal lucencies (emphysematous
spaces) which measure up to 1 cm in diameter and not bullous disease (Table II).
Table I:
Nodules distribution in both lung according to lobes
|
Nodule Site
|
Patients Number
|
%
|
|
Right Upper Lobe
|
34
|
32.3
|
|
Right Middle lobe
|
2
|
1.9
|
|
Right Lower Lobe
|
17
|
16.2
|
|
Left Upper Lobe
|
29
|
27.6
|
|
Left Lower Lobe
|
23
|
21.9
|
Table II:
Nodules Location and Lung Emphysematous status
|
|
Patient Number
|
%
|
|
Peripheral Lesion
|
83
|
79.1
|
|
Central Lesion
|
22
|
20.9
|
|
Emphysematous Changes
|
20
|
19
|
|
No Emphysematous Changes
|
85
|
81
|
Table III:
Operators and pneumothorax
|
Radiologist
|
No. of FNAB
|
No. of Pneumothorax
|
%
|
|
A
|
67
|
15
|
22.3
|
|
B
|
5
|
0
|
0
|
|
C
|
11
|
2
|
18
|
|
D
|
22
|
2
|
9
|
Four Radiologist were included in the study, two consultants (A, B) and two specialists (C, D). Majority of cases were done by A.
Nineteen patients had pneumothorax post CT-guided FNAB (18%), of which 10 were right sided (52.6%) and nine were left sided (47.3%). Seven patients
(36.8%) were detected on the immediate stage on the CT-scan table, eight patients (42.1%) were detected on follow up chest X-ray and four patients
(21%) were not detected at time of the procedure and discovered during the follow up visit one week later in the clinic. Thirteen patients (86.6%) of
the detected patients with pneumothorax were treated with chest drain at the day of the procedure.
Out of the 19 patients who developed pneumothorax, 11 patients (57.9%) had a centrally located nodule while eight patients (42.1%) had their nodule
located peripherally. Out of 19, six patients had emphysematous changes (31.5%). The distribution of cases and post FNAB pneumothorax depending on the
operator can be seen in Table III.
One patient had bleeding post chest drain insertion and needed exploratory thoracotomy to control bleeding (ligation of intercostal artery). There was
no mortality associated with the procedure.
Discussion
CT-guided FNAB is a proven method in obtaining accurate histological diagnosis of lung nodules,(5) in which a good and proven
histological diagnosis is reached but although it is a safe procedure many complications can arise in the way. Beside from pneumothorax, hemoptysis,
air embolism, bleeding, seeding of the track and death, have all been reported and encountered.(5) Pneumothorax is the most common
complication associated with the procedure.(6) and it varies from simple pneumothorax that warrants only observation to a life
threatening tension pneumothorax that needs urgent management and chest tube placement.
Rates of pneumothorax are variable from center to center, in our study the percentage of pneumothorax was 18%, it was almost equally distributed
between right and left side. Pneumothorax rate reported in literature was to range from 8 – 61%, while 1.6 - 17% of patients needed chest drains. (7,8) Serif et al. reported pneumothorax rate of 9.7% and 30% for 20 and 14 gauge respectively.(6) Smith et
al, reported over all incidence range from 8 - 64%.(7) Chest drainage reported by Takuji et al. was 22 patients out of 24
required manual repetitive aspiration of pneumothorax and four patients required chest tubes,(8) whereas in our study 13
patients out of 19 required drainage.
Multiple predisposing factors to predict the possibility for developing pneumothorax post CT-guided FNAB were studied, still none gave a definite clear
cut cause relationship.(9) Associated lung condition and diseases like emphysema and bullous disease of the lung were considered one
of the leading factors. Intra-parenchymal lesions and deeply seated lesions were the lung parenchyma had to be trespassed to reach the lesion is also
considered, the site of the lesion had no impact on the rate of pneumothorax. In our study neither the location of the nodule, nor the lung condition
had a major effect on predicting post FNAB pneumothorax.
Human factor and experience played a role in choosing the more direct way to reach the lesion and so could have played a role in predisposing to
pneumothorax as the amount of lung tissues that has to traversed by the needle and so the proportional increase of the possibility of developing lung
tissue injury and pneumothorax.
The detection of the pneumothorax was the role of the radiologist in the immediate stage and the treating doctor (Pulmonologist or Thoracic Surgeon) in
the late phase and follow ups. Missed pneumothorax were at the rim (less than 3% of lung space) and could inflect conservational treatment if detected
at time of the procedure.
Limitation of the Study
The study sample was small to give major conclusions and guidelines, secondly it was a retrospective study and there were no national data or studies
to compare with.
Conclusion
Pneumothorax post CT-guided fine needle aspiration is still a common complication in our center which had no definite single contributing factor to it,
more studies should be conducted to clarify the contributing factors to reduce its incidence.
Acknowledgment
We would like to thank Dr. Mohammad Tarshihi for his help and support.
References
1. Jordan Cancer Registry. Cancer Mortality. Cancer Incidence in Jordan 2009, 96 - 97.
2. Jaklitsch MT, Jacobson FL. The American Association for Thoracic Surgery guidelines for lung cancer screening using low-dose computed
tomography scans for lung cancer survivors and other high-risk groups. The Journal of Thoracic and Cardiovascular Surgery 2012; 144:1:33-38.
3. Baldwin DR, Eaton T, Kolbe J, et al. Management of solitary pulmonary nodules: how do thoracic computed tomography and guided fine
needle biopsy influence clinical decisions? Thorax 2002; 57:817–822.
4. Priola AM, Priola SM, Cataldi A, et al. Diagnostic accuracy and complication rate of CT-guided fine needle aspiration biopsy of lung
lesions: A study based on the experience of the cytopathologist. Acta Radiol 2010 Jun;51(5):527-33.
5. Gangopadhyay M, Chakrabarti I, Ghosh1 N, Giri A. Computed tomography guided fine needle aspiration cytology of mass lesions of lung: Our
experience. Indian Journal of Medical and Paediatric Oncology 2011; 32:4:192-196.
6. Beslic S, Zukic F, Milisic S. Percutaneous transthoracic CT guided biopsies of lung lesions; fine needle aspiration biopsy versus core
biopsy. Radiol Oncol 2012; 46(1): 19-22.
7. Smith K. Fine needle aspiration of lung lesion: lateral and Transpectoral approach. Biomed
Imaging Interv J
2011; 8(1):e2
8. Yamagami T, Nakamura T, Iida S, et al. Management of pneumothorax after percutaneous ct-guided lung biopsy. Chest 2002;
121:1159–1164.
9. Lorenz J, Blum M. Complications of percutaneous chest biopsy. Semin Intervent Radiol 2006; 23:188-193.
10. Carrafiello G, Fontana F, Mangini M, et al. Percutaneous transthoracic needle biopsy of pulmonary nodules under XperGuide cone-beam
CT guidance. MEDICAMUNDI 54/3 2010.
11. Manhire A, Charig M, Clelland C, et al. Guidelines for radiologically guided lung biopsy. Thorax 2003 58: 920-936.
12. Birchard KR. Transthoracic needle biopsy. Seminars in Interventional Radiology 2011:28:1:87-97.