ABSTRACT
Objective: To investigate the difference in effectiveness of Eutectic Mixture of Local Anesthetics (EMLA) and Benzocaine as a topical anesthetic in palatal injection
Methods: Forty volunteers from dental department at Prince Ali Bin Al Hussein Military Hospital participated in the study. 5% EMLA cream or 20% Benzocaine gel were applied to either side of the hard palate opposite the maxillary first premolars. A short needle was inserted at site of topical anesthetic application at 3, 6 and 9 minutes until it touches the bone and the volunteers assisted the pain on a visual analogue scale (VAS) where 0 indicated "no pain" and 10 indicated "unbearable pain"
Results: EMLA found to be associated with less pain than Benzocaine at all applied times and the difference was statistically significant (p < 0.05). There was no significant difference between inter-groups of EMLA or between those of Benzocaine. EMLA found to be associated with less VAS values than Benzocaine and the difference was statistically significant
Conclusion: 5% EMLA was more effective than 20% Benzocaine gel as a topical anesthetic agent in palatal injection.
Key words: Benzocaine, EMLA, Pain,Topical Anesthetic, VAS
JRMS Aug 2017; 24(2): 41-47 / DOI: 10.12816/0039641
Introduction
Pain management during dental treatment is extremely paramount. It is unfortunate that fear of pain from dental treatments persisted despite advances in pain control modalities.(1) In a survey of Japanese students in the US Domoto et al, 1991, 50% related their dental fear to needle phobia.(2) Discomfort caused by the injection is one of the main complaints of dental patients (3)and is the only uncomfortable part of any dental procedure.(4)
Clinicians, on the other hand, employ techniques to reduce pain and anxiety associated with dental injections.(5) Placement of topical anesthesia is considered the most important step to avoid pain associated with dental injections. (6)
Palatal anesthesia is important in allowing pain-free manipulation of the soft tissues on the palatal side of the tooth.(7) Palatal mucosa is tightly bound to its underlying periosteum and has abundant nerve supply, which renders injections extremely painful (8) and more resistant to the effects of topical anesthetics than any other intraoral sites (9) thus considered the optimal site to test the efficacy of topical anesthetics.(10)
Many topical anesthetics were tested but there was no agreement on their effectiveness due to individual variations, application procedure, or concentration,(11,12) however, psychological factors aid to increase the pharmacological efficiency of topical anesthesia. (5) Benzocaine is an ester type anesthetic that has been widely used since 1903.(13) It is very insoluble in water, and as such is indicated for topical applications. It is used on nasal, oral, and orotracheal mucosa.(14) It has a rapid onset and short duration effect.(15) Eutectic mixture of local anesthetics (EMLA) is a compound, which melt at lower temperatures than any of its components, permitting higher concentrations of anesthetics for use. It is composed of two amide type local anesthetics formed of 25 mg/mL of lignocaine, 25 mg/mL of prilocaine. (16) It has been used in dermatology, sinus puncture, (17) venous cannulation, (18) minor operations on the gingival tissues (19) and in reducing discomfort of rubber dam clamp(20) Although EMLA was effective in reducing injection pain, however, there is a need to develop better topical anesthetics for use on the palatal mucosa.(11) Topical anesthetics like 20% benzocaine have pharmacological and psychological effects and minimize the possible adverse effects of injections.(21) When applied locally, 20% benzocaine significantly reduces pain values obtained, but clinical relevance of the reduction is not obvious(22) The purpose of this in vivo study is to compare the effectiveness of two topical anesthetics before palatal injection in a clinically relevant application time.
Methods
Subjects
Forty volunteers (24 male and16 female aged 20 years and above) were recruited. They were the staff of the Dental Department at Prince Ali Bin Al Hussein Military Hospital. All participants had natural dentition, with no palatal or oral anomalies or pathologies, no extracted first premolar, no oral trauma or known allergy to topical or local anesthetics and not taking drugs that depress the central nervous system. The experimental protocol was approved by the Royal Medical Services Ethics Committee. A written informed consent was signed by each participant.
Pain assessment
Pain experience could be evaluated by a reliable, subjective, self reporting Visual Analogue Scale (VAS), VAS consisted of a 100 mm line with the left end (0) of which indicates “no pain” and the right end 10 indicates “unbearable pain”.(23) Before the experiment was started, VAS was explained for each participant to mark on the scale the degree of pain felt after each needle insertion.
Experiment
The experiment was conducted by a single operator, who was trained to position the needle insertion. The participants were blind to the formulations applied as they were asked to close their eyes during application of topical anesthesia. During the experiment, each participant was set in an upright position with the assistant holding the suction tip to prevent swallowing of any of the topical anesthetics. Before topical anesthesia application, the palatal mucosa was dried with a sterile gauze. 5% EMLA (AstraZeneka, UK) or Ultracre (20% benzocaine w/v Ultradent, USA) were applied randomly on either side, palatal to the maxillary first premolar between gingival margins 10 mm toward midline using a cotton swab (Citoswab, China) (Fig. 1). After 3 minutes of application, the first insertion was done using short needle gauge 27 (Tg Ject Sterilized Disposable Dental Needles, UK) 3mm from the free gingival margin to one side with bevel facing towards the bone till the needle contacts the bone then the needle was immediately removed followed by its insertion into the opposite site. The participant rated the degree of pain on the VAS. A second insertion using another needle after 6 minutes, 6mm from the gingival margin and now beginning on the opposite site of the first insertion and the degree of pain on VAS was also rated. A third new needle was used and inserted after 9 minutes at 9mm from gingival margin. No submucosal injection of local anesthetic was administered as the study was limited solely to pain caused by the insertion of the needle. Topical anesthesia was not removed until the last insertion where sterile gauze was used to remove the topical anesthetics from the palate that was rinsed with a water syringe.
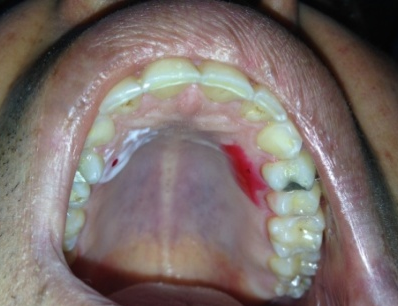
Fig. 1: Application of EMLA Cream (White) and Benzocaine Gel (Red) on palatal mucosa.
Results
The participant pool was made up of 24 males and 16 females whose ages ranged from 24 to 47 years, with an average age of 29.4 years. Based on the study design, each patient received 3 injections on each side of the palate. The mean VAS score and standard deviation for the Benzocaine group at 3 minutes was 4 and Standard deviation SD was 2.124, at 6 minutes the mean was 4.225 and SD was 2.166, at 9 minutes the mean was 3.675 and SD was 2.379 while those of EMLA at 3 minutes were 3.00 for the mean and SD was 2.038, at 6 minutes the mean was 2.85 and SD was 2.178 and at 9 minutes the mean was 2.15 and SD was 2.213. The VAS means (average) scale show that at all times (3, 6, 9) minutes were statistically significant between the two groups (Benzocaine versus EMLA), VAS scale was significantly higher among Benzocaine group (p-value < 0.05), with t-test and p-value in red color (Table I.) When benzocaine and EMLA were compared at all measured times, the mean VAS was statistically lower among the EMLA group Table II. There was no statistically significant difference between groups in Benzocaine (Table III) or EMLA (Table IV). There was no significant difference between males and females either for Benzocaine or EMLA. There was no correlation between age and VAS in both groups
Table I: The VAS means (average) at 3, 6, 9 minutes between two groups Benzocaine versus EMLA
|
|
Sig.
(2-tailed)
|
Mean
|
Std. Error
|
|
pain scale at 3
minutes-VAS
|
0.035
|
1.000
|
.465
|
|
pain scale at 6
minutes-VAS
|
0.006
|
1.37500
|
.48574
|
|
pain scale at 9
minutes-VAS
|
0.004
|
1.52500
|
.51383
|
Table II: Difference between Benzocaine and EMLA compared at all measured time.
|
|
Sig. (2-tailed)
|
Mean
|
Std. Error
|
|
BENZOCAINE VERSUS EMLA at all measured time
|
.000
|
1.30000
|
.28261
|
|
.000
|
1.30000
|
.28261
|
Table III: Difference at 3, 6, 9 minutes in Benzocaine group
|
|
Mean Square
|
Sig.
|
|
Between
Groups
|
3.058
|
.541
|
|
Within
Groups
|
4.955
|
|
|
Total
|
|
|
Table IV: Difference at 3, 6, 9 minutes in EMLA group
|
EMLA
369
|
Mean Square
|
Sig.
|
|
Between
Groups
|
8.233
|
.172
|
|
Within
Groups
|
4.600
|
|
|
Total
|
|
|
Discussion
Hamilton 1995 define needle phobia as a formal medical condition affecting approximately 10% of population and associated with avoidance behavior and physiologic changes in blood pressure, heart rate, electrocardiogram (ECG), and stress hormone. (24) This study was performed to investigate the difference in effect of using two topical anesthetics at a clinically relevant time. In this study, the needle injection after application of topical anesthetics was done at 3, 6 and 9 minutes. These selected times to examine the effectiveness of topical anesthesia were different than other studies that varied between 2-20 minutes. (3,12) Three injections only were chosen because it was easier to convince the participants of 3 injections on each side. On the other hand, the time range selected in this study was less than 10 minutes which according to the manufacturer of benzocaine used in this study (Ultracre, Ultradent, Utah, USA) is its effective time. A study by Al Melh and Andersson 2007 used 5 needle injections on each side which ended by 10 needle injections on both sides and did not clarify the site of each injection and how to avoid overlapping injections . (25) In this experiment, not only 3 injections were 3 minutes apart but also 3 millimeters distance from each other toward midline of the palate, by this technique, more time was given for the participant to rest and more time for the topical anesthetics to work with no possibility for overlapping the place of needle injection which might give the participants better chance to judge pain scores. The whole study was performed by one trained specialist to avoid personal differences and for easier repeatability for the locations of needle injections in each participant. Participants were blinded to the topical anesthetics used. There was no difficulty in application of either agent, however; it was noticed that the flow of benzocaine was more than that of EMLA which might give more advantage to the handling properties of EMLA. On the other hand, EMLA had less bitter taste and lack of odor, its ability to be applied to different areas of the oral cavity easily and in needed amounts . (25) In this study, for each injection, a new needle was inserted until it reached the bone. By this mean needle’s blunting from frequent injections will be avoided. The start site was changed alternatively at the next injection time. The measurement of pain scale used in this experiment is the visual analogue scales (VAS) which was validated as a ratio scale to measure both chronic and experimental pain (26) and has been demonstrated to be a reliable method for pain measurement (27) The present study showed that 5% EMLA application before needle injection was significantly more effective than 20% benzocaine gel in reducing pain which was in agreement with other studies that compared both topical anesthetics in maxillary vestibular mucosa (25) and in palatal mucosa.(28,29) Other studies compared EMLA to placebo and concluded that EMLA was efficient in reducing discomfort caused by the dental dam clamp in children (20) and suggested its use during gingival probing (30) or in minor operations on the gingival tissues (19) or during periodontal debridement. (30)
Although EMLA is intended for skin use and need to be occluded for 1-2 hours for optimum results, (31) the result of this study and previous studies (19,20,29,30,32) found EMLA to be a good topical anesthetic agent when applied to different sites of the oral cavity even to the palate with thick mucosal attachment and for time as short as the time used in this study of 3-9 minutes. On the other hand Primosch and Rolland-Asensi (33) compared 5% EMLA to 20% benzocaine and did not recommend the use of EMLA before palatal injection in children. In this study the feeling of anesthesia continues in some candidates for approximately half an hour even after removing EMLA cream from the palate by sterile gauze and the use of water/air spray for efficient rinsing the hard palate for any remnants of the cream. This might indicate the ability of EMLA to be easily absorbed by the mucosa of the hard palate.
While the application of topical anesthetics as 20% benzocaine was found to be effective in many studies.(34,35,36,37) Others found that the use of topical anesthetic for the inferior alveolar nerve block and posterior maxillary infiltration injections did not reduce the pain of needle insertion.(38) Hutchins et al 1997 found no difference between topical anesthetic and placebo when local solution was injected.(22) Some studies found no difference between placebo and Benzocaine even after 20 minutes of application (Fukayama et al 2002).(12) In another randomized controlled study, by Freiras et al, 20% Benzocaine was ineffective in areas supplied by the posterior superior alveolar nerve or greater palatine nerve (3) which was in agreement with theresults of this study were area supplied by the greater palatine nerve had significantly less VAS values when 5% EMLA was used rather than 20% benzocaine and at all application times. However, this might be due to the different application sites which according to Nakanishi et al 1996 was variable (39) and also might be due to the fact that some investigators gave local anesthetics after the needle injection (Hutchins et al 1997).(22)
The result of this study found no statistically significant difference between different application time either with EMLA or Benzocaine which was in agreement with Bhalla et al (2009)(40) who found no difference between 2, 5 , 10 minutes of benzocaine topical application. Although statistically insignificant, the results of this study found less pain scores with application time of 6 minutes and even much less scores when injections were made at 9 minutes either when Benzocaine or EMLA were used.
Clinically, the less effective time of topical anesthetics application would be more convenient for both the dentists and patients, however, with the VAS scores of this study, the authors recommend a time longer than 3 minutes as a topical anesthesia application time whenever possible.
Martin et al, (1994) concluded that there is at least a psychological if not a pharmacological benefit of topical anesthetic use thus making dental injection experience less traumatic because patients anticipate less pain from upcoming needle injections (5)
Meechan et al, 2002 referred to several double-blind, placebo controlled trials in their conclusion that topical anesthetics have a pharmacologic effect and they considered the different results of different studies to be due to the agent used, the application time and site of topical anesthetic application in the oral cavity.(7)
Conclusion
The use of topical anesthesia between dentists in Jordan has not been studied but there is no consensus about its routine use before needle injection. It’s the authors’ opinion that topical anesthetics should be used routinely in dental clinics in Jordan. In general there is no contraindication to the use of topical anesthetics in dentistry unless there is a known allergy to that specific anesthetic agent; however, there are some known case reports about adverse effects after the use of cetain anesthetics. Most adverse effects to the use of topical anesthesia in dentistry are associated with the occurrence of methemoglobinemia.(41-44) None of the participants experienced any adverse effect however, as explained earlier, some participants have a retained anesthetic effect half an hour after effective cleaning of the site of application of EMLA however, there are some case reports of methemoglobinemia induced by Benzocaine spray,(41) 20% Benzocaine home use(42) allergic contact dermatitis to Benzocaine (43) or contact dermatitis to EMLA cream.(44)
References
1. Dionne RA, Gordon SM, Mccullagh LM, Phero JC. Assessing the need for anesthesia and sedation in the general population. J Am Dent Assoc 1998 Feb 28; 129(2):167-73.
2. Domoto P, Weinstein P, Kamo Y, Wohlers K, Fiset L, Tanaka A. Dental fear of Japanese residents in the United States. Anesth Prog 1991 May; 38(3):90.
3. De Freiras GC, Pozzobon RT, Blaya DS, Moreira CH. Efficacy of Benzocaine 20% Topical Anesthetic Compared to Placebo Prior to Administration of Local Anesthesia in the Oral Cavity: A Randomized Controlled Trial. Anesth Prog 2015 Jun; 62(2):46-50.
4. Koppolu P, Mishra A, Swapna LA, Butchibabu K, Bagalkokar A, Baroudi K. Comparison of efficacy among various topical anesthetics: an approach towards painless injections in periodontal surgery. Saudi J Anaesth 2016 Jan;10(1):55.
5. Martin MD, Ramsay DS, Whitney C, Fiset L, Weinstein P. Topical anesthesia: differentiating the pharmacological and psychological contributions to efficacy. Anesth prog 1994;41(2):40.
6. Strazar AR, Leynes PG, Lalonde DH. Minimizing the pain of local anesthesia injection. Plast Reconstr Surg 2013 Sep 1; 132(3):675-84.
7. Meechan JG. Intra-oral topical anaesthetics: a review. J dent 2000 Jan 31;28(1):3-14.
8. Mcardle BF. Painless palatal anesthesia. The Journal of the American Dental Association 1997 May 1;128(5):647.
9. Meechan JG. Effective topical anesthetic agents and technique s. Dental Clinics. 2002 Oct 1;46(4):759-66.
10. Gill CJ, Orr DL. A double-blind crossover comparison of topical anesthetics. J Am Dent Assoc 1979 Feb 28;98(2):213-4.
11. Franz-Montan M, de Paula E, Groppo FC, Silva AL, Ranali J, Volpato MC. Liposomal delivery system for topical anaesthesia of the palatal mucosa . Br J Oral Maxillofac Surg 2012 Jan 31;50(1):60-4.
12. Fukayama H, Suzuki N, Umino M. Comparison of topical anesthesia of 20% benzocaine and 60% lidocaine gel. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2002 Aug 31;94(2):157-61.
13. Sveen OB, Yaekel M, Adair SM. Efficacy of using benzocaine for temporary relief of toothache. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1982 Jun 30;53(6):574-6.
14. Ganzberg S, Kramer KJ. The use of local anesthetic agents in medicine. Dent Clin North Am 2010 Oct 31;54(4):601-10.
15. Mura P, Maestrelli F, González-Rodríguez ML, Michelacci I, Ghelardini C, Rabasco AM. Development, characterization and in vivo evaluation of benzocaine-loaded liposomes. Eur J Pharm Biopharm 2007 Aug 31;67(1):86-95.
16. Shrinivas TR, Kumar R. Comparative evaluation of efficacy of EMLA cream (eutectic mixture of local anesthetic) and a placebo (normal saline) in producing dermal analgesia for venous cannulation. India J Clin Anesth 2015;2(1):27-31.
17. Joki-Erkkilä VP, Kääriäinen J, Penttilä M, Rautiainen M. Local anesthesia with EMLA cream for maxillary sinus puncture. Ann Oto Rhinol Laryl 2002;111(1):80-2.
18. Speirs AF, Taylor KH, Joanes DN, Girdler NM. Anaesthetics: A randomised, double-blind, placebo-controlled, comparative study of topical skin analgesics and the anxiety and discomfort associated with venous cannulation. Br Dent J 2001 Apr 28;190(8):444-9.
19. McMillan AS, Walshaw D, Meechan JG. The efficacy of Emla® and 5% lignocaine gel for anaesthesia of human gingival mucosa. Br J Oral Maxillofac Surg 2000 Feb 29;38(1):58-61.
20. Lim S, Julliard K. Evaluating the efficacy of EMLA topical anesthetic in sealant placement with rubber dam. Dermatol Surg 2004 Nov 1;26(6):497-500.
21. Deepika A, Chandrasekhar Rao R, Vinay C, Uloopi KS, Rao VV. Effectiveness of two flavored topical anesthetic agents in reducing injection pain in children: A comparative study. J Clin Pediatr Dent 2012 Sep 1;37(1):15-8.
22. Hutchins Jr HS, Young FA, Lackland DT, Fishburne CP. The effectiveness of topical anesthesia and vibration in alleviating the pain of oral injections. Anesth Prog 1997;44(3):87.
23. Franz-Montan M, de Paula E, Groppo FC, Ranali J, Volpato MC. Efficacy of liposome-encapsulated 0.5% ropivacaine in maxillary dental anaesthesia. Br J Oral Maxillofac Surg 2012 Jul 31; 50(5):454-8.
24. Hamilton JG. Needle phobia: a neglected diagnosis. J Fam Pract 1995 Aug 1; 41(2):169-76.
25. Al-Melh MA, Andersson L. Comparison of topical anesthetics (EMLA/Oraqix vs. benzocaine) on pain experienced during palatal needle injection. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007 May 31; 103(5):16-20.
26. Price DD, McGrath PA, Rafii A, Buckingham B. The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain. 1983 Sep 1; 17(1):45-56.
27. Price DD, Bush FM, Long S, Harkins SW. A comparison of pain measurement characteristics of mechanical visual analogue and simple numerical rating scales. Pain. 1994 Feb 28;56(2):217-26.
28. Abu AM, Andersson L, Behbehani E. Reduction of pain from needle stick in the oral mucosa by topical anesthetics: a comparative study between lidocaine/prilocaine and benzocaine. J Clin Dent 2004 Dec;16(2):53-6.
29. Singh S, Jayanth BS, Gupta K. Diminution of Pain from Needle Insertion in Palatal Mucosa By Two Topical Anaesthetics: A Comparative Study Between Lidocaine/Prilocaine (EMLA) and Benzocaine. J Adv Med Dent Scie Res 2015;3(3):9-15.
30. Donaldson D, Gelskey SC, Landry RG, Matthews DC, Sandhu HS. A placebo‐controlled multi‐centred evaluation of an anaesthetic gel (Oraqix®) for periodontal therapy. J Clin Periodontol 2003 Mar 1;30(3):171-5.
31. Kuwahara RT, Skinner RB. EMLA versus ice as a topical anesthetic. Dermatol Surg 2001 May 1;27(5):495-6.
32. Donaldson D, Meechan JG. A comparison of the effects of EMLA cream and topical 5% lidocaine on discomfort during gingival probing. Anesth prog 1995; 42(1):7.
33. Primosch RE, Rolland-Asensi G. Comparison of topical EMLA 5% oral adhesive to benzocaine 20% on the pain experienced during palatal anesthetic infiltration in children. Pediatr Dent 2001;23(1):11-4.
34. Rosivack RG, Koenigsberg SR, Maxwell KC. An analysis of the effectiveness of two topical anesthetics. Anesth prog 1990 Nov; 37(6):290.
35. Svensson P, Petersen JK. Anesthetic effect of EMLA occluded with Orahesive oral bandages on oral mucosa. A placebo-controlled study. Anesth prog 1992; 39(3):79.Vickers ER, Punnia‐Moorthy A. A clinical evaluation of three topical anaesthetic agents. Aust Dent J 1992 Aug 1;37(4):266-70.
36. Al-Samadani KH, Gazal G. Effectiveness of benzocaine in reducing deep cavity restoration and post-extraction stress in dental patients. Saudi med J 2015 Nov;36(11):1342.
37. Nusstein JM, Beck M. Effectiveness of 20% benzocaine as a topical anesthetic for intraoral injections. Anesth prog 2003;50(4):159.
38. Nakanishi O, Haas D, Ishikawa T, Kameyama S, Nishi M. Efficacy of mandibular topical anesthesia varies with the site of administration. Anesth prog 1996; 43(1):14.
39. Bhalla J, Meechan JG, Lawrence HP, Grad HA, Haas DA. Effect of time on clinical efficacy of topical anesthesia. Anesth Prog 2009; 56(2):36-41.
40. Hegedus F, Herb K. Benzocaine-induced methemoglobinemia. Anesth Prog 2005;52:136–139.
41. Chung NY, Batra R, Itzkevitch M, Boruchov D, Baldauf M. Severe methemoglobinemia linked to gel-type topical benzocaine use: a case report. J Emerg Med 2010; 38(5):601-606.
42. González-Rodríguez AJ, Gutiérrez-Paredes EM, Fernández ÁR, Jordá-Cuevas E. Alergia de contacto a benzocaína. Importancia de los resultados positivos concomitantes en las pruebas epicutáneas. Actas Dermosifiliogr 2013; 104(2):156-8.
43. Waton, J., Boulanger, A., Trechot, P. H., Schmutz, J. L. and Barbaud, A. Contact urticaria from Emla® cream. Contact Derm 2004: 51(5‐6):284-287.